Acetaminophen is one of the most common pain relievers in the world. You’ll find it in dozens of products-from cold medicines to prescription painkillers like Vicodin. But what most people don’t realize is that taking just a few extra pills can turn a routine dose into a life-threatening situation. Acetaminophen overdose is the leading cause of acute liver failure in the U.S., and many cases happen because people think they’re being careful.
How Much Is Too Much?
The recommended maximum daily dose for adults is 4,000 milligrams. That sounds like a lot-until you realize how easy it is to hit that limit. A single Extra Strength Tylenol tablet has 500 mg. If you take two every four hours, you’re already at 3,000 mg by the end of the day. Add a prescription painkiller like Vicodin (which contains 300 mg of acetaminophen per tablet), and you’re over the limit before lunch.
Some people take extra pills because their pain isn’t gone. Others don’t know their cold medicine already contains acetaminophen. A 2022 study found that nearly 70% of people who overdosed didn’t realize they were doubling up. The liver doesn’t care if you meant to take too much. It only sees the chemical overload.
What Happens in Your Liver?
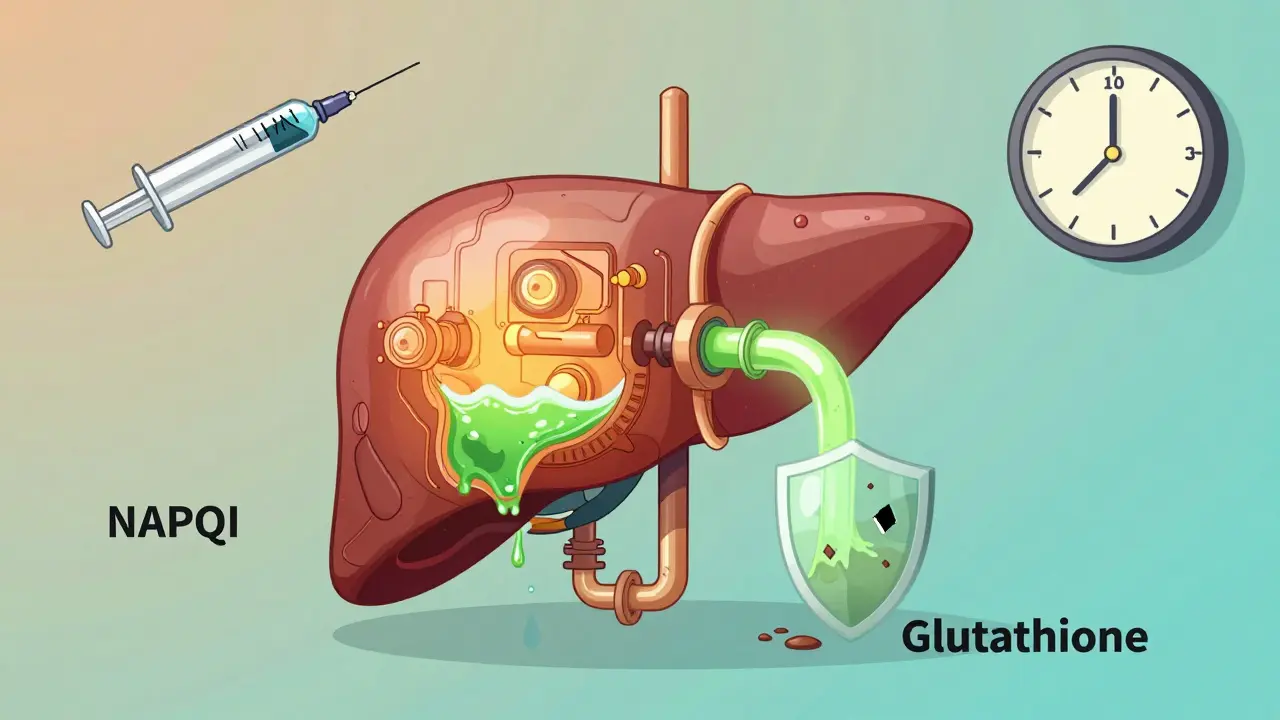
Your liver breaks down acetaminophen using enzymes. Most of it becomes harmless waste. But about 5-10% turns into a toxic byproduct called NAPQI. Normally, your liver uses glutathione-a natural antioxidant-to neutralize it. But when you take too much acetaminophen, your glutathione runs out. NAPQI starts attacking liver cells, causing massive damage.
This isn’t a slow process. It happens fast. The damage begins within hours. By the time you feel sick, your liver may already be failing.
The Four Stages of Toxicity
Acetaminophen poisoning follows a clear timeline. Knowing these stages can save your life-or someone else’s.
Stage 1 (0-24 hours): You might feel fine. Or you might get nauseous, vomit, or lose your appetite. About 40% of people show no symptoms at all. This is the most dangerous stage because you think you’re okay. But inside, your liver is already under attack.
Stage 2 (24-72 hours): The pain starts. Right side of your abdomen becomes tender. Nausea returns. Your liver enzymes begin to climb. ALT levels-the key marker for liver damage-start rising. Normal is under 56 IU/L. In overdose cases, they can jump past 10,000 IU/L. That’s like a siren going off inside your body.
Stage 3 (72-96 hours): This is the crisis. Jaundice appears-your skin and eyes turn yellow. You feel confused. Your blood doesn’t clot properly (INR over 1.5). Kidneys start to fail. About half of people with severe liver damage also develop kidney problems. At this point, death is possible without treatment.
Stage 4 (5+ days): Recovery or death. If you got help in time, your liver can regenerate. Around 85-90% of people who get treated early bounce back fully. Without treatment, the death rate jumps to over 25%.
The Only Antidote: N-Acetylcysteine (NAC)
There’s one treatment that works: N-acetylcysteine, or NAC. It’s not a miracle drug-it’s a lifeline. NAC works in two ways: it replaces the glutathione your liver lost, and it binds directly to NAPQI, stopping the damage.
Timing is everything. If you get NAC within 8 hours of taking too much, it’s 98% effective. After 8 hours, effectiveness drops by 25%. At 15 hours, it’s barely half as effective. Every hour counts.
The standard IV dose is given over 21 hours: 150 mg/kg over the first hour, then 50 mg/kg over four hours, then 100 mg/kg over the next 16 hours. Oral NAC is an option too, but it takes 72 hours and often causes vomiting, making it harder to keep down.
Even if you show up 24 hours later, NAC still helps. Studies show it reduces death rates even when given up to 48 hours after overdose. Don’t wait. Don’t assume you’re fine because you don’t feel sick.
What Else Do Hospitals Do?
When you arrive at the ER, they don’t just give you NAC. First, they check your blood level of acetaminophen. If it’s above 150 µg/mL at the 4-hour mark, you get NAC immediately. That’s based on the Rumack-Matthew nomogram-a chart doctors use to predict risk.
If you took the pills less than two hours ago, they might give you activated charcoal. It traps the drug before your body absorbs it. But after two hours, it’s too late.
They’ll also give you fluids to keep your kidneys working. Anti-nausea meds like ondansetron. Vitamin K or plasma if your blood won’t clot. And they’ll monitor your liver enzymes, kidney function, and blood pH constantly.
Who’s at Highest Risk?
Not everyone who overdoses gets liver damage. Some people are far more vulnerable.
- Chronic alcohol users: Drinking regularly lowers glutathione levels and speeds up toxin production. Risk increases 3-4 times.
- People with hepatitis B or C: Their livers are already damaged. Overdose risk jumps 65%.
- Those on seizure meds: Drugs like carbamazepine or phenytoin speed up how fast your liver turns acetaminophen into poison. Risk goes up 40%.
- Malnourished people: Low protein intake cuts glutathione by 25-30%. This includes people with eating disorders, the elderly, or those with chronic illness.
If any of these apply to you or someone you care for, be extra cautious. Even one extra pill can be dangerous.
When Do You Need a Liver Transplant?
For a small number of people, the damage is too severe. About 1-2% of overdose cases end in acute liver failure. When that happens, doctors use the King’s College Criteria to decide if a transplant is the only option.
You’re at risk if:
- Your blood pH is below 7.3 (too acidic)
- Your INR is above 6.5 (blood won’t clot)
- Your creatinine is over 3.4 mg/dL (kidneys failing)
If you meet two or more of these, survival without a transplant is nearly zero. With a transplant, 85% live at least five years. But you need to be referred fast-transplant centers don’t wait.

What Happens After You Recover?
Most people who survive an overdose get their liver back. Around 92% have full liver function within three months. But 8% keep seeing slightly elevated liver enzymes. That means ongoing monitoring is needed.
Long-term, you should avoid acetaminophen completely. Your liver may be more sensitive. Even normal doses could be risky. Talk to your doctor about alternatives like ibuprofen or naproxen-but only if your kidneys are healthy.
How to Prevent Overdose
Most overdoses aren’t intentional. They’re mistakes. Here’s how to avoid them:
- Check every medicine label. Acetaminophen is listed as “APAP” or “acetaminophen.” If two products have it, don’t take them together.
- Never take more than 4,000 mg in 24 hours. Some experts now recommend 3,000 mg max for safety.
- Don’t use acetaminophen for more than 10 days straight without seeing a doctor.
- If you drink alcohol regularly, skip acetaminophen entirely.
- Keep medicines out of reach of children. A single 500 mg tablet can be deadly for a kid.
- If you’re unsure, ask your pharmacist. They can check all your meds in seconds.
In 2011, the FDA forced manufacturers to reduce the maximum single dose in prescription pills from 750 mg to 500 mg. That change alone cut liver failure cases by 21% over 10 years. Education works.
What’s New in Treatment?
Researchers are looking for better ways to treat overdose. One promising area is nitric oxide. Early studies in mice and zebrafish show it helps the liver regenerate-even after the damage has started. This could mean NAC doesn’t need to be given so early. But it’s still experimental.
Another breakthrough? Blood tests for microRNA-122. This tiny molecule spikes within 2 hours of liver damage. In trials, it’s 94% accurate at detecting acetaminophen injury before symptoms appear. Imagine an at-home test that tells you if you’ve taken too much. That’s the future.
Right now, though, the rule is simple: if you think you’ve taken too much, go to the ER. Don’t wait. Don’t call a friend. Don’t hope it’ll pass. Get NAC.
Can you overdose on acetaminophen by taking too many cold pills?
Yes. Many cold, flu, and sinus medicines contain acetaminophen. Taking one Tylenol on top of a cold tablet can push you over the 4,000 mg limit. Always check the active ingredients. If it says "acetaminophen" or "APAP," you’re getting it. Don’t combine products.
Is it safe to take acetaminophen if you drink alcohol occasionally?
Occasional drinking (once or twice a week) with normal doses of acetaminophen is usually safe for healthy adults. But if you drink regularly-even just a few drinks a week-your liver is more vulnerable. Avoid acetaminophen altogether if you drink daily. The risk isn’t worth it.
What if I took too much acetaminophen but feel fine?
Feeling fine doesn’t mean you’re safe. The first 24 hours after an overdose often show no symptoms. Liver damage can be silent until it’s too late. If you took more than 7.5 grams (15 extra-strength tablets), go to the ER immediately-even if you feel fine. Waiting even 6 hours can triple your risk of severe liver damage.
Can NAC be given at home?
No. NAC is a medical treatment that requires monitoring. IV NAC can cause allergic reactions like low blood pressure, rash, or breathing trouble. Oral NAC causes severe nausea and vomiting. Neither should be self-administered. Only hospitals have the equipment and staff to manage side effects and ensure proper dosing.
How long does it take for the liver to heal after an overdose?
Most people recover fully in 3 months. Liver cells regenerate quickly if the damage isn’t permanent. Blood tests for liver enzymes (ALT, AST) usually return to normal within 1-2 weeks. But you should avoid alcohol and acetaminophen for at least 6 months. Some people need lifelong monitoring if they had severe damage.

Tom Sanders
March 10, 2026 AT 22:52Philip Mattawashish
March 12, 2026 AT 22:00Jazminn Jones
March 14, 2026 AT 00:59Stephen Rudd
March 14, 2026 AT 18:08Robert Bliss
March 16, 2026 AT 06:28Peter Kovac
March 18, 2026 AT 00:39Judith Manzano
March 19, 2026 AT 20:55rafeq khlo
March 19, 2026 AT 22:08Morgan Dodgen
March 20, 2026 AT 07:53APRIL HARRINGTON
March 20, 2026 AT 21:17Leon Hallal
March 22, 2026 AT 11:54Neeti Rustagi
March 23, 2026 AT 12:10Ray Foret Jr.
March 24, 2026 AT 14:13Samantha Fierro
March 25, 2026 AT 22:54Erica Santos
March 26, 2026 AT 10:11