Spine Inflammation: Causes, Treatments, and How Medications Help
When your spine inflammation, inflammation of the spinal structures that leads to pain, stiffness, and reduced movement. Also known as spinal inflammation, it can stem from injury, autoimmune disorders, or long-term wear and tear. It’s not just a sore back—it’s your body’s immune system reacting in ways that can damage joints, discs, or nerves over time. If you’ve been told you have spine inflammation, you’re not alone. Millions deal with it every year, often without knowing what’s really going on inside.
Common triggers include corticosteroids, medications used to reduce inflammation in conditions like arthritis or spinal stenosis, which can help—but only if used correctly. Long-term use can lead to skin thinning or bone loss, as shown in studies on topical and oral steroids. Then there’s anti-inflammatory meds, drugs like NSAIDs that block pain signals and reduce swelling in the spine. These are often the first line of defense, but they don’t fix the root cause. And if you’re on multiple prescriptions, you need to watch for interactions—like how magnesium can interfere with osteoporosis drugs, or how nasal sprays like Rhinocort work differently than oral steroids.
What you’ll find in the posts below aren’t generic tips. They’re real, practical insights from people who’ve been there: how to track if your meds are working after a switch, why using one pharmacy cuts your risk of dangerous mix-ups, and how to spot when a steroid is doing more harm than good. You’ll see how spine inflammation connects to other conditions—from autoimmune disorders to muscle spasms linked to neurological issues—and what treatments actually move the needle. No guesswork. No marketing fluff. Just what works, what doesn’t, and what your doctor might not tell you.
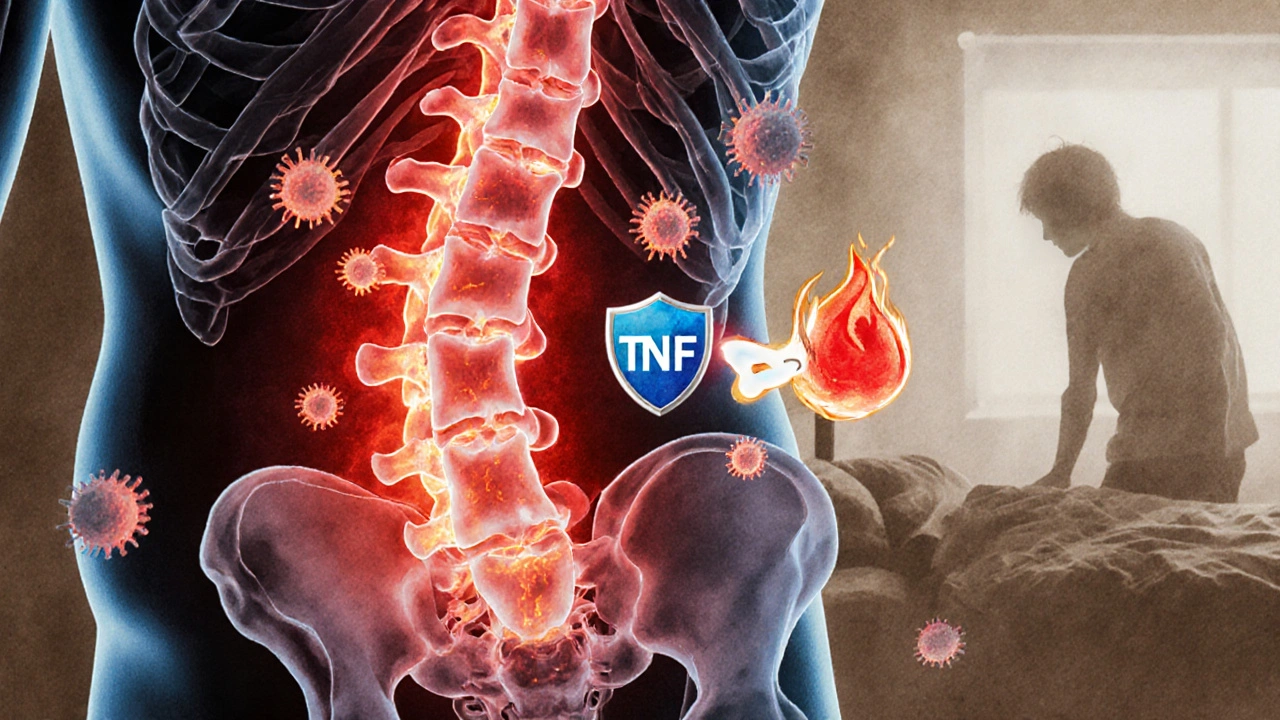
Ankylosing Spondylitis: How TNF Inhibitors Reduce Spine Inflammation and Improve Mobility
Ankylosing spondylitis causes chronic spine inflammation that can lead to fusion and disability. TNF inhibitors block the key driver of this inflammation, offering significant relief and slowing disease progression for most patients when started early.
November 9 2025